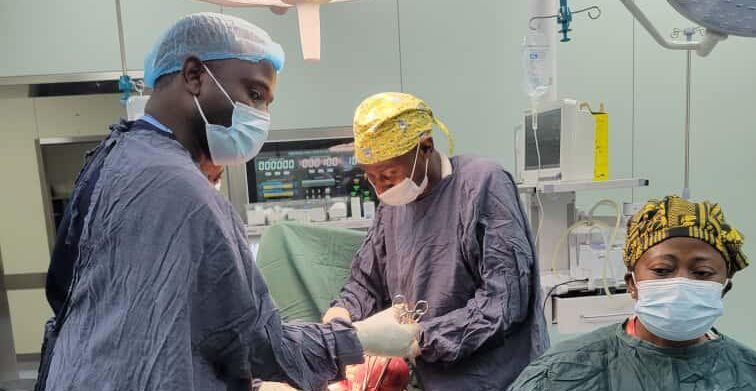
When we encounter data on maternal and newborn mortality, it is tempting to see these as only numbers. Yet, the statistics translate into families torn apart, a diminished workforce, and the loss of precious lives that would have fueled our regional development. This reality compels me to ask a key question: Why do maternal, newborn, and sexual and reproductive health (SRH) outcomes remain so poor in the ECSA region despite having proven solutions? Is the barrier a lack of knowledge or is it a critical shortage of skilled specialists exactly where they are most needed?
It is vital to first recognize that these deaths are entirely preventable. In answering the question of why they persist, we must acknowledge that maternal and newborn mortality, alongside unmet SRH needs, are driven primarily by a critical shortage and unequal distribution of specialist obstetricians and gynaecologists., Too many rural and underserved facilities still lack the specialized providers required to manage obstetric emergencies and deliver comprehensive SRH services.
In many countries in the region, specialists are concentrated in urban referral hospitals, leaving rural and underserved populations without access to advanced care. As a result, women in these settings often deliver in facilities without skilled personnel to manage life-threatening complications such as postpartum hemorrhage, obstructed labor, or pre-eclampsia.
Similarly, newborns face fragile survival odds without experts to treat sepsis or respiratory distress. These delays in care and the lack of expertise continue to cost lives, not because the medicine doesn’t exist, but because the specialists do not.
The answer lies in training specialist obstetricians and gynecologists directly within the region’s own health systems, a mission the East, Central and Southern Africa College of Obstetrics and Gynaecology (ECSACOG) is currently spearheading. By training specialists where they are most needed, ECSACOG ensures that education is context-relevant, strengthens ownership, and builds sustainable capacity. These experts do more than provide lifesaving care; they mentor fellow health care providers and fortify the entire health system’s capacity to handle emergencies.
Through structured residency programme, which is conducted in accredited training sites, and supported by standardized examinations, ECSACOG is producing specialists who are well equipped to lead and teach. These specialists are critical to the health system: they manage complicated cases, provide comprehensive SRH servicesand strengthen referral systems.
However, training alone is not enough. There are broader challenges related to retention and overburdened specialists in referral centers who must juggle clinical care, trainee supervision, and administration. There is an urgent need for increased investment, stronger political commitment, and expansion of accredited training institutions to scale up the workforce.
The question is not whether specialist training works, the evidence is clear that it does. The real question is whether we are investing at a scale that matches the burden of maternal, newborn, and SRH challenges in the region. Strengthening ECSACOG is not optional; it is a strategic priority and a cornerstone of resilient health systems. It is an investment in survival, equity, and dignity for women, newborns, and adolescents across the ECSA region.